Last updated on March 22, 2019

One of the first things a girlfriend of mine asked when I told her I was pregnant was whether or not I would give birth without painkillers. It was one of the first glimpses I had of the pressure that women face about giving birth. A natural, non-medicated birth tends to be held up as a beacon of goddess-like triumph. And my hat is off to all the women who achieve it. I know it’s not an easy route and it’s one that certainly takes courage. But a natural birth is also a privilege and I think it’s wrong that so many of the women who have medical intervention during birth are left feeling as though they failed or achieved something lesser than those who didn’t. After all, every birth is a triumph. And varying circumstances, bodies and minds mean that the options are different for everyone.
My birth story
When I first found out I would likely have to have a caesarean, I stepped out of the doctor’s office and cried on Steve’s shoulder, feeling instant grief for the birth that I had imagined. For months I’d been preparing for a natural delivery, going to antenatal classes and practising hypnobirthing techniques. I was excited more than scared and I looked forward to the intensity of the experience. I guess I wanted to be that goddess.
But prior medical issues with my pelvic floor meant that I was eventually advised to have a caesarean. If I didn’t, it was likely I’d need surgery afterwards or, worse, that there would be complications with the delivery. No-one could say for sure what the outcome would be and I was given advice not firm instructions, so I had to make the final decision myself. There were lots of things to weigh up, from the pluses and minuses of natural/caesarean birth to the consequences if things didn’t go smoothly. My consultant had told me that the worst option for my pelvic floor would be an instrumental delivery, but that’s not something that’s easily avoided if you need it in the moment. The whole decision-making process was a string of ‘what ifs’, nothing certain and all options with their own risks. So in the end, we made a compromise: we booked a date for an elective caesarean, but if I went into labour before then, I planned to see how labour was progressing and potentially try it naturally.
This meant I continued to prepare for both a natural birth and a caesarean right up until the day Otis was born. In a way this wasn’t weird as all births could end up either way regardless of your situation, so I think it’s wise to prepare for both. However as the date of our elective neared, I knew my chances for a natural birth were slimming. I did all the things to try and speed things up, from eating dates to trying acupuncture, but nothing seemed to work. In hindsight, I think that was for the best.

Preparing for a c-section
We booked the elective about three weeks in advance, but we kept the date a secret as we still wanted the birth to be a surprise for our loved ones. In the UK, electives tend to be done at 39 weeks because any earlier than that ups the likelihood of the baby having breathing difficulties, and any later means you get increasingly likely to go into spontaneous labour and potentially need a less calm, emergency c-section. We booked ours for 39 weeks plus three days, on 23 January.
One week before the op we had an appointment at the hospital where a nurse and an anaesthetist talked us through what would happen on the day and the things we needed to do to beforehand. There were meds (antacids and anti-sickness) I needed to take the night before and the morning of, plus a glucose drink to have beforehand. I needed to fast from midnight, so the glucose drink kept me going before the op at 8am. A benefit of an elective is that you have the chance to take these precautions that help the operation go nice and smoothly.
We made a birth plan for the caesarean that outlined all our wishes. Happily, everything we wanted was in line with our hospital’s standard procedure. They deliver babies slowly, which helps to squeeze fluid from the lungs as would happen in a vaginal delivery. They delay the cutting of the cord, so the baby gets that extra placental blood. The baby is placed on the mother’s chest almost immediately for that special skin-to-skin bonding. And they encourage breastfeeding as soon as possible. All of these elements were things I was worried about missing out on because of having a c-section instead of a natural birth, so it was reassuring to know that the hospital was already on the same page. It’s not that long ago that caesareans were all done under general anaesthetic so the mother would be unconscious for the whole thing. In this case, I’d be fully awake and Steve would be there beside me.

We were also allowed to play our own music during the operation, which entailed hours of agonising over the perfect playlist and trying fruitlessly to time what would be playing when he was actually born! In the end it was a song by Einuadi followed by some Edward Sharpe. The surgical team complimented us on our choices as just the week before they’d been subjected to Ed Sheeran on repeat!
The night before the elective had the feeling of Christmas Eve when as a child you can’t sleep for the excitement. We knew when we closed our eyes that the next morning would be our son’s birth date. I held my belly and sent messages of strength to the baby that had grown inside it. It felt beyond comprehension that tomorrow we would meet him.
The next morning, after some final bump photos and a shower, Steve and I drove to the hospital with our empty baby car seat and carefully packed overnight bag, filled with things I’d never needed before, like giant knickers and lanolin cream. We were headed out for our most monumental trip yet. I’d never had surgery before, so I was unsure what to expect. My main concern was that the spinal block wouldn’t work and I’d have to have a general anaesthetic instead. I was desperate to be conscious for the delivery.
Once at the hospital, we were shown to the recovery room where the staff all came to introduce themselves – the surgeon, midwife, anaesthetist and nursing assistant. They talked through what their role was and read through our birth plan. We couldn’t have felt in better hands.

The operation
With Steve in scrubs and me in a fetching open-backed gown, we made our way to the theatre. “Welcome to our office” smiled the anaesthetist and kept up a jolly banter as things got started. I was given my spinal injection, which gave no more than a short-lived stinging pain and feeling of warmth as the anaesthesia began to take hold. It was an odd sensation as I began to lose the feeling in my legs, but a relief to know it was working. A canula was also placed in my hand and I was hooked up to a drip. The anaesthetist had control of this during the operation, regularly checking in to see if I felt light-headed or nauseous and the meds needed adjusting.

Once the anaesthesia was fully working from the chest down, tested by a spray of freezing cold water, the operation could begin. Steve was by my side, with the anaesthetist at the other. There was a curtain between my chest and the surgeons, so I was shielded from the more gory side of things. But I did request they lower it a little when Otis was born, so I could see him as soon as possible. The anaesthetist also talked us through all that was happening, again at my request. Despite being numb during the op, you can still feel that something’s happening. It’s most commonly described as feeling like someone’s doing the washing up inside of you, and to be honest that’s pretty accurate!
The whole atmosphere was calm and despite being in a brightly lit theatre, I still felt in a protective bubble, anchored by my eyes on Steve.
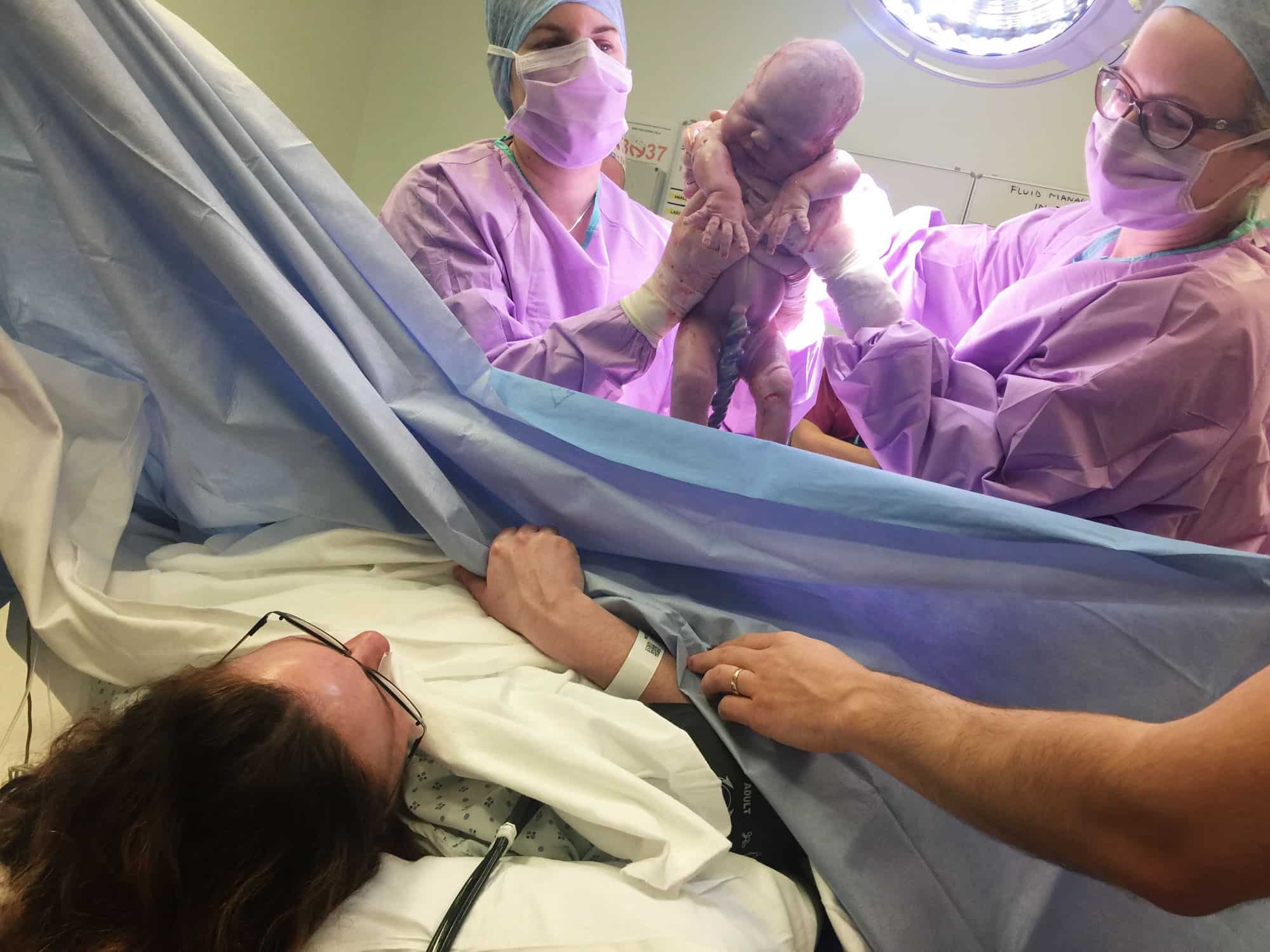
The birth
It was only around five minutes into the operation that the anaesthetist turned and said they were ready to reach for our baby. He lowered the curtain and within seconds I heard the best sound that’s ever reached my ears – the wail of our son’s first cry. My sense of relief was huge – he was here, alive and breathing. Our son had entered the world.

After a moment, Otis’ cord was cut and he was very briefly taken to the side of the room to be checked and weighed by the midwife before being placed upon my chest. For me, there’s never been a more magical moment: Otis stopped crying as soon as he was on me and that’s where he stayed for the remainder of the operation, curled up on my chest as Steve and I gazed at him in awe. I didn’t even notice when they finished stitching me up.

After the operation
While I was transferred from the operating table to a bed, Steve got his first chance for a cuddle with Otis before he was placed back in my arms and we were wheeled back to the recovery room. This was about half an hour after he’d been born and as soon as we got there, with help from a nurse, I was able to start to breastfeed. I felt beyond high that all had gone so smoothly and that this 8lb 5oz baby was finally here and in my arms.

We spent about an hour in that recovery room, feeding Otis and having the much-celebrated post-birth cup of tea and toast, all the while just marvelling at the baby I’d just birthed.

Those early hours are blurry. I know the feeling started to come back to my legs and at some point we must have been moved to the maternity ward where we’d booked a private room. We stayed there that night and the next day, leaving in the evening. Midwives came and went, helping with our questions. I fed Otis, Steve changed his nappies and we all had lots of cuddles. I was bed bound until the next day when they removed the catheter I’d had for the operation. The hospital I was at practises what they call enhanced recovery following a c-section, which means they encourage you to get moving as soon as possible. I was out of bed the next morning, shaky on my feet but so happy to be moving and able to have a shower.

I was welcome to stay in the hospital longer, but was keen to be back at home. So once I’d been given the go-ahead and Otis had his health checks, we started to pack our bags, and 36 hours post-operation, we made our way back home. It was a painful journey with every turn and speed bump rocking my wound, but luckily we live just five minutes from the hospital, so it wasn’t too much to get through.

And then we were home, no longer two but three, and I don’t think I’ve ever felt so vulnerable. Within a couple of hours of arriving back, Otis had a scary spit up where we thought that he was choking. I was terrified by his fragility and wondered how we’d cope. But we did, and slowly over the next weeks, we learned our little one’s ways.
The recovery process

At first I was daunted by the recovery. The pain and its effect on my mobility left me yearning for it to end and I was unsure how long that would take. I scoured the internet for similar stories, but all said different things. Recovery varies for everyone. For me, the worst thing was not being able to care for Otis independently. It hurt to get up and down out of bed or off the sofa, so I relied on Steve a lot, and if Otis cried I couldn’t rush across the room to be there. But that period of time was short and I was lucky to have Steve’s help.
I’ll write more about my recovery in a separate post, but in short, by the end of week one, I had taken a 5-minute walk outside, by week two, I’d been to cafes 15 minutes’ walk away, and by week three I felt so much better. It was week four when I stopped taking painkillers and started to push the pram myself. In hindsight, my recovery was swift. It was just the uncertainty that made it feel longer.

Now, four months down the line and with Otis in my arms as I type this one-handed on my phone, the birth has faded as my mind becomes consumed by motherhood. During pregnancy, I had so much of my attention on the birth that it was hard to think about what would come after. And what came next was motherhood. No matter how you give birth – at home, in an operating theatre or in a taxi en route to the hospital, you become a mother on the other side. The disappointment I felt about my c-section came before I had it. After it all I felt was joy – joy that Otis was here and gratitude that he’d arrived so smoothly. We’re all goddesses in the end.

I’d love to hear your birth experiences too.

I loved reading this 🙂 It’s so lovely you’re going to have this on your blog so you can remember it forever. I didn’t write about my birth experiences because I thought I’d remember every detail forever but it’s gets hazy already.
I had c-sections with both my boys. George, my eldest, was breach so it was recommended I had a section and I cannot tell you the relief I felt when the doctor said that. I think I’m the opposite to most women and I loved being told this. It took so much pressure and worry off and once I knew I was having it, it made me really relax and enjoy the rest of my pregnancy.
Because I’d already had one c-section they give you the option second time around so I opted for a second one and had another similar and really positive experience. I actually enjoyed my recovery at home too. I’m not the type to ever sit still so being forced to spend the majority of the day on the sofa was actually what I needed!
Congratulations for both and God bless your baby:-D!
Thank you for this article Victoria. I loved what you said, “we’re all goddesses in the end.” I really wanted a natural delivery, but after a long and difficult labour with the baby becoming stressed, I had to have an instrumental delivery. I felt very guilty for a long time and felt I could’ve done more for our daughter. This is a comforting read, thank you. ❤️
great ! Wish you always happy
I just cried reading your story. I haven’t had a baby yet, but I can relate to this so much. I will have to a c-section once I do get pregnant, and I hate how it’s often scoffed at or viewed as something less than wonderful by so many mothers who are able to have natural births. For me, a c-section represents possibility and hope. It’s likely that I won’t even get that far, but I will definitely not give up. I’ve had 13 intestinal surgeries and other medical procedures that have left me with pretty poor chances of being able to have a baby, but if I am lucky enough to somehow make it work, a natural birth won’t be possible. And I’m completely okay with that. I’m even looking into the possibility of finding a surrogate to carry my baby for me if I’m unable to. Creating life is beautiful, and it definitely shouldn’t be viewed as some sort of competition to see who does it better. I love that you wrote a post addressing this issue and shared your vulnerability with the world. Your new family is beautiful and inspiring and absolutely perfect. <3
I came across you today on Pinterest when searching for ‘baby friendly Barcelona’ and your story was Just what I needed following a traumatic, unplanned emergency C-section with my boy (also name Otis!!). Despite it being incredibly rushed and scary, I found the surgery amazing. I now think about further children and I am very torn as to what I would opt for next time tbh. I also felt a little let-down by the whole thing, liked I’d let him down and myself… but I recon that’s definitely down to women’s perceptions of ‘an easy option!’ It’s far from it isn’t it?!!!! I feel like if I opt for elective C section next time (all being well and lucky) then I’m really missing out on a different experience, but your story seems so lovely, that at least it’s possible to have a calm, lovely experience alongside a section.
Thank you for sharing!
I’m so happy the post was useful. That’s exactly why I shared it 🙂 Good luck with whatever you decide!
I just found out I’d need an elective cesarian today after months of planning a natural drug free birth. I’m filled with grief and disappointment. But reading your story gave me so much hope. Your family is beautiful. Thank you for writing and sharing this. It means the world to me right now.
I’m so pleased it was helpful. Just know that a caesarean can be a beautiful birth too 🙂
Thank you for posting this. I’m choosing to have a c-section due to being completely terrified to have a vaginal birth. I’ve been depressed with tremendous anxiety daily. My Dr just approved me to have one… so I’m starting to look up positive c-section stories.
Im glad it wasn’t a nightmare like so many moms say.. I hope to have one similar to yours. ❤️